|
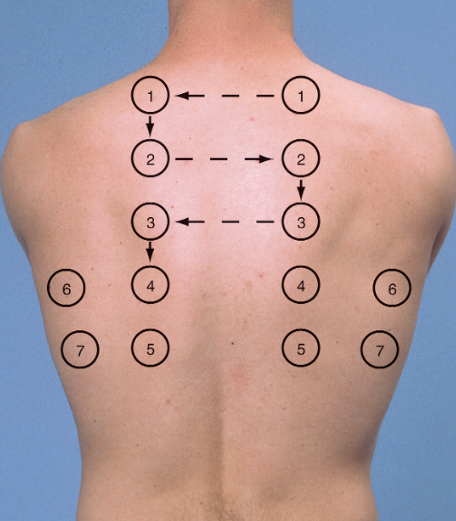
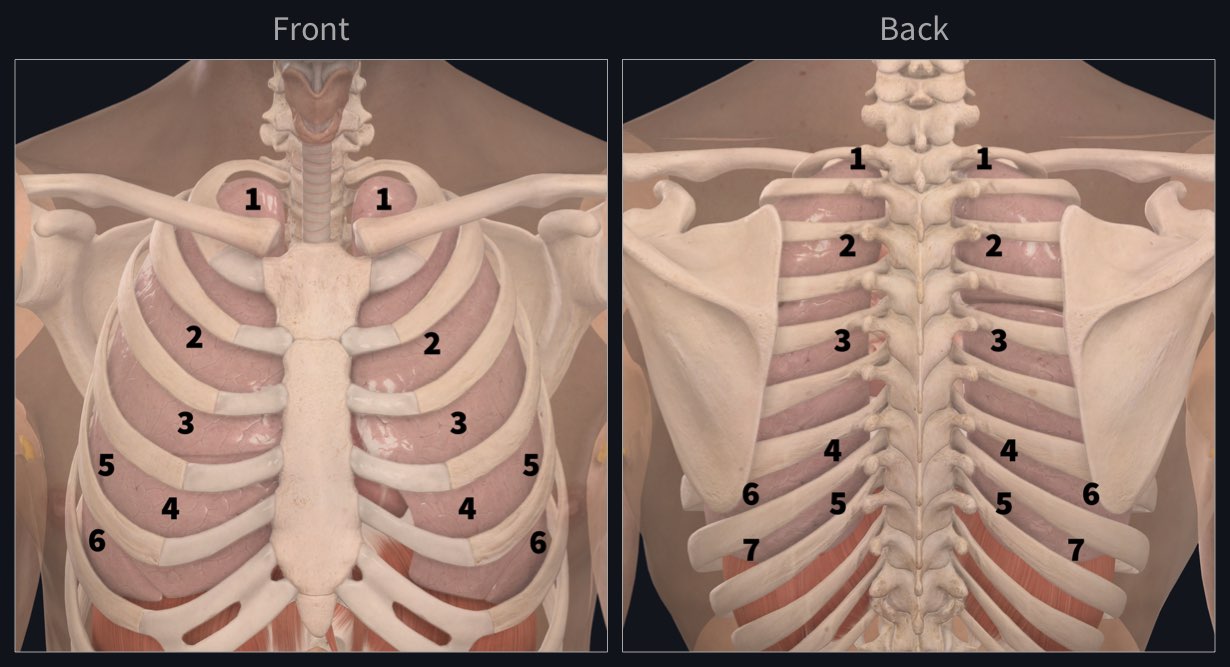
The optimal position for chest auscultation is sitting in a chair, or on the side of the bed. A chaperone should be offered for the assessment if this is considered appropriate. Listening to a patient’s chest to establish breath and any other sounds requires a quiet area, so that health professionals can fully appreciate what they hear and interpret their clinical relevance (Sarkar et al, 2015).Ĭhest auscultation requires the chest and back to be exposed, so measures should be taken to ensure the patient’s privacy and dignity is maintained at all times. Nurses need to assess individual patients for the risk of exposure to blood and body fluids (Royal College of Nursing, 2018) and to be aware of local policies for glove use. Non-sterile gloves are not required routinely for this procedure. Nurses are advised to have a stethoscope for their own use, as sharing equipment may increase infection risk and maintaining clean ear tips can be difficult. Adherence to local infection prevention and control policies, including the cleaning of equipment between every patient contact, is essential. The stethoscope is an important tool for clinical assessment, but can become contaminated by micro-organisms (Longtin et al, 2014). Fig 3 illustrates parts of the stethoscope. The bell of the stethoscope is generally used to detect high-pitched sounds – at the apex of the lungs above the clavicle its diaphragm is used to detect low-pitched sounds in the rest of the chest (Dougherty and Lister, 2015). Mid zone: level of the hilar structures. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
